A Million to One: Bridging the biomarker chasm from discovery to the clinic
21 Dec 2021
With so much research being published on biomarkers, yet so few companion diagnostic devices being cleared by the FDA, Rafael Rosengarten discusses why it is so hard to develop a biomarker to the point of clinical utility.
From the business perspective, advancing drugs into and through clinical trials is expensive and risky. Biomarkers can dramatically reduce that risk, and hasten the timeline to get drugs on the market.
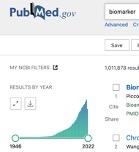
A current search of PubMed will return approximately one million entries for papers related to biomarkers, showing an exponential increase in the database since 1980 (Figure 1). However, on the same day, the FDA lists only forty-six cleared or approved companion diagnostic (CDx) devices [1]. These numbers reveal orders of magnitude difference between the current investments in biomarker research compared to available approved biomarkers for incorporation into a patient treatment plan. Why is it so hard to develop a biomarker to the point of clinical utility for patient reporting and to guide decision making?
A biomarker, plainly put, is a characteristic that is objectively measured and evaluated as an indicator of normal biological processes, pathogenic processes, or pharmacologic responses to a therapeutic intervention [2]. Biomarkers can be assessed across many categories— encompassing a broad range of measurable biological characteristics from a single chemical in the blood to the entire genome of a cancer cell. They also have many diagnostic applications. Biomarkers can be used to detect or confirm a disease state. Prognostic markers report on the risk or probability of an event, like disease progression. Drug safety, pharmacodynamics, and exposure monitoring may all be assessed by respective biomarkers. Finally, predictive biomarkers endeavour to stratify patients that are likely to respond or not respond to therapy [3]. In the context of drug development and commercialisation, predictive biomarkers are best aligned with the aim of precision medicine to match patients to the optimal therapy for their particular disease.
Biomarkers as a fundamental component of therapeutic development
Why should predictive biomarkers become a fundamental component of therapeutic development and patient treatment?
Consider that the vast majority of investigational drugs entering clinical trials fail to advance through to final approval, often being deemed safe in phase 1 but lacking efficacy in Phase 2 and 3. For example, in the therapeutic area of oncology, the overall clinical trial success rate is estimated as low as 3 - 4% [4].
Stratifying patients via the use of a biomarker aims to identify individuals whose biology better matches the mechanism of action of the therapeutic. Defining the intent to treat patient populations as those for whom the drug is most likely to be effective can increase the probability of successful regulatory approval. In a retrospective modelling study of five major cancer indications, Parker and colleagues (2021) report a 5-12x increased likelihood of progression from one clinical phase to the next for biomarker stratified trials [5]. Investigational biomarkers—those employing analytical methods that measure more biological complexity—even outperformed more traditional, approved tests.
In complex diseases, including cancer, autoimmune disorders, and viral infections such as COVID-19, predicting patient response to treatment is especially challenging. Characterising disease biology is a key step in determining the best possible therapy due to the uniqueness of individuals’ disease at the molecular level. Often it proves insufficient to measure only a single biomarker, because even when a specific causal molecular aberration is targetable, that knowledge alone may not predict the outcome of drug intervention. Thus, biomarkers that account for molecular complexity and population heterogeneity may be a more effective guide for treatment decisions.
The cutting edge of biomarker discovery
The cutting edge of biomarker discovery consists of high-throughput and multi-parametric analysis. Exciting approaches include various ‘omics, e.g., well established methods such as gene expression profiling and newer techniques like glycoproteomics.
Other evolving technologies, such as digital pathology, also promise to yield insights into disease subtypes and addressable patient populations. The challenge, and opportunity, in precision medicine is to confront biological complexity, both in terms of choosing which molecular features to measure, and in determining how to model these features for patient classification.
Data engineering as an art
Machine learning (ML) is a branch of artificial intelligence focused on training algorithms to find complex patterns in data—with or without human intervention—that humans could not identify by eye or intuition [6]. All too often, we sequence millions of DNA variants or tens of thousands of expressed gene transcripts, but only from a few dozen or a couple hundred patients in a clinical study. The resulting data matrices require a series of statistical transformations following a data quality control protocol to make them ML-ready.
Implementing the appropriate data engineering is often as much art as science. Further, organising the appropriate clinical data alone is a significant undertaking, and has inspired industry-wide initiatives to define guidelines such as FAIR (Findable Accessible Interoperable Reusable) in response to the challenge.
Precision medicine requires investment and commitment
Precision medicine programs require investment in human talent, technology, data, and education. Such commitments make sense. From the business perspective, advancing drugs into and through clinical trials is expensive and risky. Biomarkers can dramatically reduce that risk and hasten the timeline to get drugs on the market.
From a human perspective, people’s lives are at stake. If faced with a tough decision of which experimental drug to take, especially for a terminal disease for which this might be the last shot, we owe it to patients to give them the best possible chance of responding to therapy and improving their disease condition.
We now have the tools to measure and model each patient’s disease, thus we have the responsibility to do everything in our power to use that data to make the most well-informed treatment decisions. Widespread adoption of predictive biomarkers will help turn all of medicine into precision medicine.
Author: Dr Rafael Rosengarten is CEO of Genialis
References
- https://www.fda.gov/medical-devices/in-vitro-diagnostics/list-cleared-or-approved-companion-diagnostic-devices-in-vitro-and-imaging-tools
- Biomarkers Definitions Working Group. Clin Pharmacol Ther. 2001 Mar; 69(3):89-95
- Califf RM. Exp Biol Med (Maywood). 2018 Feb;243(3):213-21.
- Wong, Siah & Lo. Biostatistics. 2019; 20, 2: 273–86
- Parker JL. Cancer Medicine. 2021;10:1955–63.
- Allgood et al. The AAIH. 2019.